When living with aHUS, being prepared for complications is challenging
A look at how May-Thurner syndrome affected this patient and columnist
Written by |

When I nearly died a few years ago from a rare disease I’d never heard of, I was understandably overwhelmed. And it wasn’t only because of thoughts about my own mortality, but also all of the comorbidities that came along with the disease. I hadn’t expected that I might spend the rest of my life fighting multiple health complications.
In September 2020, I spent nearly two months in intensive care, fighting for my life. I’d developed a rare disease triggered by COVID-19 called atypical hemolytic uremic syndrome (aHUS). I was in multiorgan failure (and now have permanent damage to my kidneys, liver, heart, and uterus). While hospitalized, I had 18 blood transfusions, plus dialysis, plasmapheresis, and antibody therapy. I had an entire team of doctors taking care of me.
After I was diagnosed, I went almost immediately to Google to learn as much as I could about this disease. I also searched social media to see if anyone else had aHUS. To my surprise, I found two Facebook groups full of patients, family members, and caregivers.
I read posts and comments for hours. I had nothing but time on my hands in intensive care, so I tried to absorb as much information about aHUS as I could. Anyone who knows me understands that I always like to know what will happen next. I like to have control of a situation and plan for what’s to come. But nearly dying was something I definitely had no control over.
Online support groups and doctors helped prepare me for hypertension issues, long-term dialysis, hemolytic anemia, a long, slow recovery, and many other problems that come with aHUS. But I wasn’t prepared for the swelling that would rule my life for years to come.
Hello, edema
When I was in intensive care, nephrologists would frequently visit to touch base with me and discuss my kidney function and other issues. They always checked my ankles and feet and asked if I had any swelling. I never did, so it seemed odd that they asked me about it every day. My ankles and feet were actually smaller then normal because I was losing so much muscle mass. I was also spending up to 23 hours a day in my hospital bed.
But after I was released and went home, the swelling started. If I stood, walked, or even sat up in a chair for longer then 15 minutes, my ankles and feet would begin to swell. The most severe edema would spiral out of control in just minutes. And it got so bad that my skin started to split and bleed.
This swelling was a symptom I wasn’t prepared for. I didn’t notice many others talking about it in the Facebook groups, either. At the time, I also didn’t realize that the swelling was worse on the left side of my body. In reality, I was starting to develop another rare complication because of all the hypertension medications I was taking.
May-Thurner syndrome caused my left-side swelling to become a problem morning, noon, and night. Even when I’m resting now, my left side swells. It’s escalated so much that my blood pressure has become higher on my left side then it is on my right — a complication that needs to be addressed.
Last winter, my primary care physician changed practices, so I had to start seeing a new doctor, one who was shocked by the issues I’d been dealing with. She immediately wanted to address them, so we began adjusting my blood pressure medications to see if we could get the May-Thurner syndrome symptoms to subside.
Thankfully, after several modifications, I’m happy to report that my right side almost never swells, and most of the swelling on my left side has gone away. I still have a blood pressure imbalance, however, and healthcare workers can’t draw blood from my left arm. But I can at least walk around and do normal activities for a couple hours a day.
I wasn’t prepared for any of this when my aHUS journey began. But who can say they know what to expect when dealing with rare and chronic illnesses?
If you’re in a similar situation, it’s important to remember that quality of life matters, even if it’s not the main focus of your doctors. Keep pushing, learning, and moving forward.
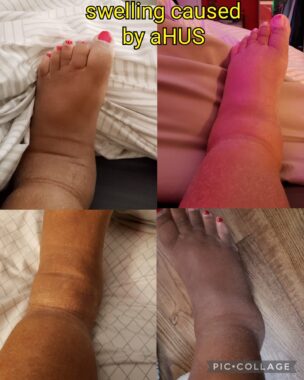
A photo collage of Shalana Jordan’s edema. (Courtesy of Shalana Jordan)
Note: aHUS News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of aHUS News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to aHUS.






Leave a comment
Fill in the required fields to post. Your email address will not be published.